Single Needle Thoracic Paravertebral Block with Ropivacaine and Dexmeditomidine for Radical Mastectomy: Experience in 25 Cases
Kalpana Rajendra R Kulkarni
DOI10.21767/2471-982X.100013
D Y Patil Medical College Kolhapur, Maharashtra, India
- *Corresponding Author:
- Kalpana Rajendra R Kulkarni
D Y Patil Medical College Kolhapur
Maharashtra India
Tel: 9822065665
E-mail: drrmk@rediffmail.com
Received date: April 20, 2016; Accepted date: November 29, 2016; Published date: December 06,2016
Citation: Kulkarni KRR. Single Needle Thoracic Paravertebral Block with Ropivacaine and Dexmeditomidine for Radical Mastectomy: Experience in 25 Cases. Int J Anesth Pain Med. 2016, 2:1. doi: 10.21767/2471-982X.100013
Abstract
Background: Currently regional technique like thoracic paravertebral block for breast surgery is gaining a lot of popularity. As it produces unilateral action thereby minimal hemodynamic changes with autonomic blockade, allows early ambulation, facilitates postoperative analgesia, eliminate the risks/complications of general anaesthesia and thus reduces the hospital stay and cost.
Aims and Objectives: We aim to present an observational prospective study to evaluate single needle continuous thoracic paravertebral block as a sole anaesthetic technique using ropivacaine 0.5% 20 ml with an adjuvant 0.5 mcg/Kg of dexmeditomidine in 25 females undergoing modified radical mastectomy.
Methods: Following thorough evaluation, Informed consent and necessary OT preparations, thoracic paravertebral space was detected using 18G Tuohy needle at the level of T 4 on the operative side in sitting position. Epidural catheter was passed 2-3 cm inside the paravertebral space and patient was made supine. Following test dose of 3 ml 1.5% lignocaine with adrenaline, 20 ml (2 ml/segment) of 0.5% ropivacaine with 0.5 mcg/kg dexmeditomidine injected through the catheter.
Results: All the patients had good to excellent surgical anaesthesia. No significant hemodynamic changes noted. Four patients required IV fentanyl 0.5-1 mcg/kg for mild discomfort intraoperatively. The level of sedation was adequate with minimal side effects. Conclusion: Single needle continuous thoracic paravertebral block using ropivacaine 0.5% with dexmeditomidine 0.5 mcg/kg as a sole anesthetic technique provided satisfactory surgical anaesthesia with minimal hemodynamic changes and adverse effects in 25 cases of radical mastectomies.
Keywords
Paravertebral block; Ropivacaine; Dexmeditomidine; Radical mastectomy
Introduction
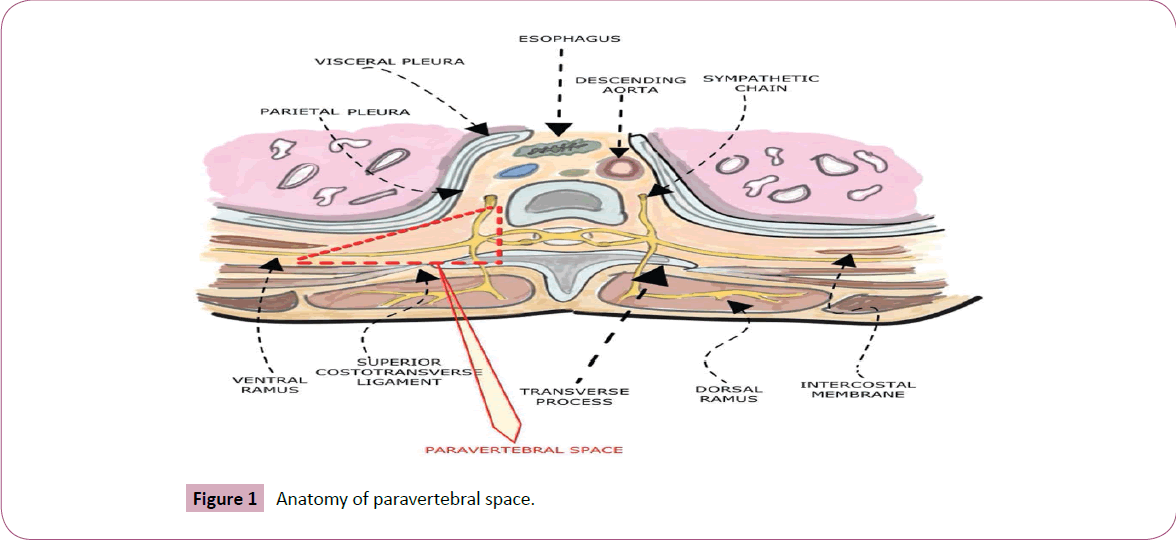
Thoracic Paravertebral Block (TPVB) was introduced by Hugo Sellheim in 1905. It was further refined by Lawen and Kappis but it became popular after the work by Eason and Wyatt who presented a reappraisal on thoracic paravertebral block [1]. The indications for paravertebral block have expanded in recent years, as more anesthesiologists have become experienced with the technique. Female mastectomies done under (TPVB) have shown that it is a promising technique, it provides comfortable surgical field than with the conventional technique of General Anaesthesia (GA). Thus it eliminate the risks and complications of GA with distinct advantage of minimal hemodynamic changes, early ambulation resulting in lesser stay and cost of the treatment [2]. Paravertebral space is a triangular wedge shaped space bounded by superior costotransverse ligament, transverse process, anterolateral parietal pleura, posteriorly intercostal membrane, medially by vertebral body, intervertebral disc and space, adjacent ribs are superiorly and inferiorly. It contains adipose tissue, spinal nerves, sympathetic chain, and intercostal vascular structures, preganglionic white and postganglionic gray rami communicants.
Paravertebral block is a technique creating unilateral somatic and sympathetic nerve block as a result of Local Anesthetic (LA) injection close to the spinal nerves along the columnavertebralis.
For breast surgery, the blocks are performed between T2 and T6 with either multiple injections or single shot/continuous technique that can be performed in sitting, lateral or prone positions [3,4]. Though it is an established technique for acute/ chronic and postoperative pain management for thoracic/ abdominal surgeries but it is less utilized as a sole regional anaesthetic technique. We aimed to present an observational prospective study of the classical technique of Loss of Resistance (LOR) using Tuohy needle for continuous TPVB with ropivacaine 0.5% and dexmeditomidine 0.5 mcg/kg as a sole anaesthetic for surgical anaesthesia in 25 patients scheduled for radical breast surgeries at our Institution since Jan 2014 (Figure 1).
Methods
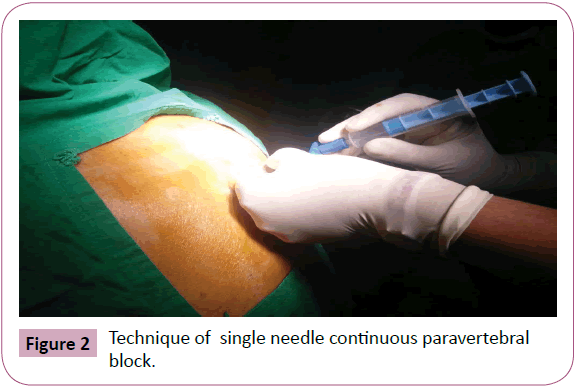
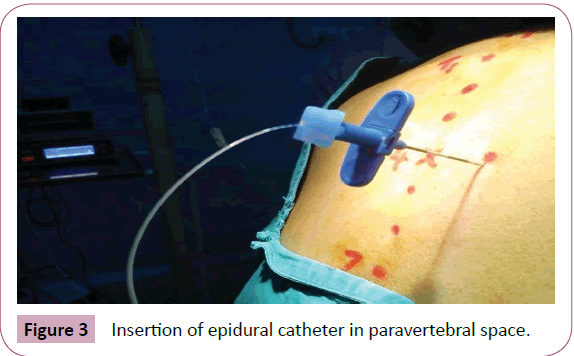
After thorough pre-anaesthetic evaluation /optimization and ethical approval, Informed consent was taken from 25 ASA grade I-III females posted for modified radical mastectomy. Patients with coagulopathy, kyphoscoliosis, severe cardiopulmonary diseases, allergic to Local Anaesthetics and refusal for regional techniques were excluded. Tab diazepam 10 mg was given at night before surgery. On the day of operation intravenous (IV) access obtained and ringer’s lactate 10 ml/kg infusion started. Premedication with IV glycopyrrolate 0.004 mg/kg was given. Vital monitoring started for ECG, PR, NIBP, SpO2 and temperature. Under aseptic precautions single needle continuous TPVB at the level of T4 on the side of operation was given as described by Eason et al. [1,4-6]. The patient was given sitting position with head and neck in flexed position. Spinous process of T 4 vertebra located and a point marked 2.5 cm lateral to it (Figure 2). Following LA infiltration of the skin and subcutaneous tissue, with the help of 18 G Tuohy needle, bevel facing upwards and using LOR technique, needle advanced perpendicularly upto 4-5 cm until it hits the transverse process, further advanced for 5-10 mm past transverse process in cephalade direction till the LOR is appreciated. An epidural catheter inserted 2-3 cm inside into the paravertebral space and patient was made supine. In case of any difficulty in catheter insertion needle rotated so as to face the bevel caudally or laterally. Figure 3, following negative aspiration test for blood/CSF, a test dose of 3 ml of 1.5% lignocaine with adrenaline injected. Five minutes later, 20 ml of 0.5% ropivacaine (2 ml per segment or 0.3 ml/kg approx.) with 0.5 mcg/kg of dexmeditomidine (in increments of 10 ml) injected through the catheter in paravertebral space. Sensory block was assessed bilaterally by pin prick method every 5 minutes to note the extent of block and for development of parasthesia on opposite side. If no parasthesia in any of the desired dermatomes it was considered as a failed block. The maximum extent of block was expected to be between C7- to T 10 dermatomes for radical mastectomy. The hemodynamic monitoring was done continuously for pulse rate, noninvasive blood pressure, oxygen saturation (SpO2), electrocardiography ECG ,temperature and blood loss.
Intraoperative sedation achieved with a dose of midazolam 1 mg IV. Any discomfort or rise in pulse rate or mean blood pressure more than 20% was managed with IV 0.5-1 mcg/kg of fentanyl. Nasal oxygen supplementation with 3 litres of flow was given throughout the operation. Postoperative assessment for pain on VAS (0-10) score, sedation score (0-No sedation, I-mild, IImoderate, III-deep sedation), duration of analgesia that is time for first request for analgesic was noted (VAS>3) when top up dose of ropivacaine 0.2% 10 ml injected through the catheter in the paravertebral space. Later top ups repeated every 6 hourly. Requirement of rescue analgesics (Inj. Tramadol 100 mg IV) and side effects like nausea vomiting, breathlessness or any other, noted for first 24 hours. Assessment of restricted arm movements on 0-III score (0-No pain, I-mild restriction, II-moderate restriction, III-severe restriction) was noted every 6 hourly.
Statistical analysis
In Table 1 demographic parameters like age, height, weight, blood loss, duration of surgery are mentioned as mean values +/- SD of respective units and as number of patients in each type of ASA grade. In Table 2 block parameters like time to perform block, onset time and time to complete block, depth of skin to paravertebral space, intra operative pulse rate, mean blood pressure, oxygen saturation, blood loss, post operative VAS score and duration of analgesia are mentioned as mean values +/- SD of respective units. Rest of the parameters are mentioned as number of patients in each grade or group and median values for dermatomal block and range of sedation score. The data was entered in MS Excel sheet and basic data analysis tool park is used for analysis.
Results
The demographic profile of the patients is shown in Table 1. There were 25 ASA grade I-III patients of carcinoma breast. Mean duration of surgery was 90 minutes. Table 2 depicts the anesthesia parameters of the patient. The time required for performing the block was 15(10) minutes. The depth of insertion of the needle to reach the paravertebral space was 5(1) cm. Onset time of sensory block was noted and it was 5(3) minutes. Time to maximum effect that is from injection of the drug into the paravertebral space till maximum block of dermatomes 8(7-10) is achieved and it was 15(7) minutes. No parasthesia was observed contralaterally.
| Parameters | Values (mean+/-SD, numbers) |
| Age | 58(10)yrs |
| Weight | 70(15)kg |
| Height | 150(10)cm |
| ASA Class(I/II/III) | 5/12/8 |
| Type of Surgery | Radical mastectomies |
| Duration of Surgery | 90(20) min |
Table 1: Demographic Profile
| Parameters | Values (Mean +/-SD, Median,Range,numbers) |
| Time to perform block | 15(10) minutes |
| Depth of skin to paravertebral space) | 5 ( 1) cm |
| Onset timeof sensory block | 5(3) minutes |
| Time to complete block | 15(7)minutes |
| Median Dermatomes blocked | 8(7-10) |
| (Intraoperative) Pulse Rate | 90(12)/min |
| Mean Blood Pressure | 100(10)mm of Hg |
| Oxygen Saturation (SpO2) | 100(5)% |
| Number of Pts. requiring IV Supplementation of fentanyl | 4 |
| Blood loss | 130(30) ml |
| Post operative mean VAS | 2(1) |
| Sedation score | I-II |
| Duration of Analgesia | 360(60) minutes |
| No. of rescue analgesics in 24 hours | 2(3 patients) |
| Respiratory depression | 0 |
| Restricted Arm Movements (0/I/II/III) | 0/22/3/0 |
| PO Nausea/ Vomiting | 2/1patients |
Table 2: Summary of anesthesia related parameters.
Intraoperatively there were no significant changes (>20%) in the pulse rate or mean blood pressure and oxygen saturation (SpO2) when compared to the base line and it was within normal range. No incidence of bradycardia, hypotension or desaturation occurred intraoperatively. Four patients required supplementation of IV fentanyl 50-100 mcg in increments of 25 mcg for mild discomfort during dissection towards midline and axillary clearance. Blood loss during surgery was 130 (30) ml. Postoperative pain relief was adequate and the first top up analgesic dose was given by injecting 10 ml of ropivacaine 0.5% through the catheter in the paravertebral space when (VAS>3) at around 360 (60) minutes that was considered as duration of analgesia. Rescue analgesia was provided with Inj.tramadol 100 mg IV if VAS>3, that needed in 3 patients within 24 hours. No patient complained of breathlessness intra or post operatively and SpO2 was maintained in the range of 95 to 100%. Sedation score was observed in the range of I-II. Restricted arm movements in the post operative period was observed of grade 0-0/ I-22/ II-3/III-0 patients. Postoperatively nausea/ vomiting occurred in 3 patients, they responded well to Inj.ondesetrone 4 mg and ranitidine 50 mg IV.
Discussion
General anaesthesia for radical breast surgery is considered to be gold standard. However it is associated with increased incidence of nausea-vomiting, postoperative pain and increased need of paranteral opioids. Post operative restricted and painful shoulder movements delay ambulation, prolongs the hospital stay and thus precludes ambulatory breast surgery [5]. TPVB is indicated as a primary anaesthetic technique for simple chest wall surgeries, rib resection and for breast augmentation surgeries. More often it is utilized as an analgesic for breast carcinoma surgery, minimally invasive cardiac surgery, post thoracotomy pain, multiple rib fractures, acute herpetic neuralgia and other chronic pain conditions. Pusch et al. reported effective anaesthesia with single injection of high volume of bupivacaine in TPVB for breast lump excision and mastectomies with axillary clearance [4-6]. Richardson et al. suggested TPVB is a safe and effective technique and should be considered as an ideal alternative to general anesthesia for unilateral thoracic surgeries [7,8]. LA like bupivacaine 0.0625% or ropivacaine 0.2% at the rate of 3-10 ml/hour in infusion form are found very effective in providing post operative analgesia [9]. The other regional method of choice for breast surgery is thoracic epidural anaesthesia which is effective and prolonged postoperative analgesia can be provided however it is associated more with technical difficulty, risk of neurological damage, postural hypotension due to autonomic blockade, urinary retention and hence limits mobilization/ambulatory discharge. With TPVB there is minimal risk of neurological damage, being unilateral with sympathetic blockade incidence of postural hypotension is less unless the patient is hypovolemic and thus ambulatory discharge is possible. Patient’s satisfaction is better as compared to thoracic epidural or general anaesthesia with lesser hospital stay and cost of treatment hence TPVB is considered as a safe alternative to epidural anaesthesia [3,4,8]. Davies et al. in his meta-analysis found similar efficacy of pain relief with epidural and TPVB however failure rates and incidence of complication reported significantly higher in thoracic epidural group [8]. Richardson et al. reported similar results with better preservation of postoperative pulmonary functions and effective coughing in TPVB as compared to thoracic epidural [9,10]. Single needle catheter technique of TPVB has been used to provide surgical anaesthesia for breast surgeries and shown that LA spreads 1-4 dermatomes cephalic and upto 7 dermatomes caudally with 15 ml of 1.5 mg/kg 0.5% bupivacaine [2,5,6,9,11,12]. We too observed a good spread over 7-10 thoracic dermatomes with 20 ml of 0.5% ropivacaine with dexmeditomidine 0.5 mcg/kg when injected through catheter. There was good hemodynamic stability where no patient developed significant hypotension, bradycardia or desaturation. Incidence of nausea occurred in 2 and vomiting in 1 patient and the results are similar to the studies by others [3,11].
The complications and side effects reported with TPVB are very low and varies from 2.5-5 % amongst them hypotension 4.6%,vascular puncture 3.8%, pleural puncture 1.1% pneumothorax 0.5% and no mortality reported [5,8,9]. In our study there was no incidence of pleural puncture or pneumothorax in any patient and no supplementation with GA required. IV analgesia with 0.5- 1 mcg/kg of fentanyl needed in four patients for mild discomfort intraoperatively. On radiological evaluation epidural spread has been reported by Beyaz et al. resulting in bilateral local anaesthetic effects in a case of radical mastectomy conducted under TPVB [4]. Failure rates with TPVB is <13%. Naja and Lonnqvist reported 6.1% failure following TPVB when studied in 620 adults and 42 children [12,13]. LOR with air/saline is a common method of detecting paravertebral space and variety of LA like bupivacaine, ropivacaine, levobupivacaine with adjuvants like adrenaline, opioids, alfa 2 agonists are used successfully. There are reports of successful use of sole TPVB for surgery in male gynecomastia and for breast surgeries in high risk patients like having ischemic heart disease, obstructive cardiomyopathy, myasthenia gravis and even in pregnant patient for cancer breast surgery [14-19]. Exadaktylos et al. [19] mentioned in his retrospective study on 129 patients of breast cancer surgery about significant reduction in tumor recurrence and metastatic spread when performed under regional technique of TPVB because of reduced stress response, improved immune functions, decreased release of inflammatory substance-P and suppressed neurokinin-1 over expression of tumor cells [4] reported better results when GA was combined with TPVB for pain control and Poleshuck et al. noted that 40% of the patients of breast cancer surgery are poorly managed for perioperative pain and suffers from chronic pain. TPVB provides good postoperative pain control and protects these patients from developing chronic pain significantly [2,20]. Variety of LA used includes bupivacaine or levobupivacaine from 0.25-0.5%, ropivacaine 0.5-1% as analgesic with GA or sole TPVB for breast cancer surgeries [4,11,15]. Hura et al. compared the efficacy 0.5% bupivacaine with 0.5% ropoivacaine for radical mastectomies under TPVB and found rapid onset with ropivacaine with longer lasting analgesia and wider spread over 9 segments as compared with bupivacaine. However analgesic efficacy was equipotent in both the groups [21].
Yoshida et al. studied the effect of 0.2% and 0.5% ropivacaine on segmental spread after continuous TPVB and found no significant difference related to the concentration used [22]. We too observed sensory block of 7-10 segments with 20 ml of 0.5% ropivacaine. Alfa 2 agonist like clonidine and dexmeditomidine are used as an adjuvant for neuroaxial and perineural anaesthesia and well reported for TPVB [15,23]. Mohamed et al. compared the effects of addition of dexmeditomidine 1 mcg/kg to 0.25% of ropivacaine in TPVB for modified radical mastectomies. They observed significant intraoperative hemodynamic stability prolonged postoperative analgesia and decreased need of rescue analgesics for 48 hours after surgery [23]. In our study with 0.5% ropivacaine and 0.5 mcg/kg dexmeditomidine we found similar results of hemodynamic stability with postoperative analgesia of mean 6 hours with lesser need of rescue analgesics (3/25 patients in 24 hours postoperatively) . Nerve stimulator guidance to improve the needle-nerve position or ultrasound guidance increases the accuracy and efficacy of TPVB, thus minimizes the incidence of side effects or complications [2,9,12,14,15].
Ultrasonography is useful to guide the needle tip into the thoracic paravertebral space,visualize the catheter and drug spread allowing lesser volume of LA that minimize the risk of complications like accidental intravascular injection, pleural puncture or pneumothorax and thus improves the therapeutic success [24-26]. Although less practiced USG guidance is currently recommended but availability of ultrasound, adequate training and development of skill is required.
Limitations
Although GA is gold standard for breast cancer surgery, it is associated with certain complications and currently TPVB is also an established technique but less utilized. Hence we followed the protocols laid down by other studies [1,2,5,6,9,11,12] and conducted study in breast cancer surgeries under sole TPVB. We also found satisfactory results proving its effectiveness as a sole regional technique that supports the studies mentioned in the article. The limitations with our study is that the sample size is small and we have not compared the TPVB with GA or other regional technique like thoracic epidural block. We aimed to evaluate the classical technique of paravertebral block using LOR with Tuohy needle. Due to nonavailability ultrasound guidance was not considered in our patients. Further study is needed in more number of patients with the use of nerve stimulator or USG guidance which is known to improve the efficacy of block. Also we need to compare other techniques of anaesthesia for cancer breast surgery, so as to confirm the superiority of TPVB.
Conclusion
In our study single needle continuous TPVB was effective as a sole technique to provide surgical anaesthesia for radical mastectomies in 25 patients. There were minimal hemodynamic changes, side effects and it facilitated post-operative analgesia.
Conflicts of Interest
The authors declare that there is no conflict of interests regarding the publication of this paper.
Acknowledgement
We acknowledge the support of Asso. Professor Dr Sheetal Murchite (Dept. of Oncosurgery, D Y Patil Medical College, Kolhapur) for the support while conducting this study.
References
- Eason MJ, Wyatt R (1979) Paravertebral thoracic block‑ a reappraisal. Anaesthesia 34: 638-642.
- Schnabel A, Reichl SU, Kranke P, Pogatzki-Zahn,Zahn PK (2010) Efficacy and safety of paravertebral blocks in breast surgery: A meta-analysis of randomized controlled trials BJA 105: 842-852.
- Coveney E, Weltz CR, Greengrass R, Iglehart JD, Leight GS, et al. (1998) Use of Paravertebral Block Anesthesia in the Surgical Management of Breast Cancer. Experience in 156 Cases. ANNALS OF SURGERY 4: 496-501.
- Beyaz SG, Ergönenç T, Altıntoprak F, FuatErdem A (2012)Thoracal paravertebral block for breast surgery. Dicle Med J 39: 594-603.
- Karmakar MK (2001) Thoracic paravertebral block. Anaesthesiology95:771-780.
- Pusch F, Freitag H, Weinstabl C(1999) Single-injection paravertebral block compared to general anaesthesia in breast surgery. ActaAnaesthesiolScand43: 770-804.
- Richardson J, Sabanathan S (1995) Thoracic paravertebral analgesia. ActaAnaesthesiolScanda39: 1005-1015.
- Davies RG, Myles PS, Graham JM(2006) A comparison of the analgesic efficacy and side-effects of paravertebral vs epidural blockade for thoracotomy--a systematic review and meta-analysis of randomized trials. Br J Anaesth96: 418-426.
- King K, Kelly JE (2012) Paravertebral Blocks: The Evolution of a Standard of Care.Pain Medicine News Special Edition Dec MCMOHAN Publishing pp: 69-77.
- Richardson J, Sabanathan S, Jones J, Shah RD, Cheema S, et al.(1999) Aprospective, randomized comparison of preoperative and continuous balanced epidural or paravertebral bupivacaine on post-thoracotomypain, pulmonary function and stress responses. Br J Anaesth83:387-392.
- Koh D,KhaiL (2013) The Use of Single-injection Thoracic Paravertebral Block in Breast Cancer Surgeries in our Asian Population: The Singapore General Hospital Experience. Proceedings of Singapore Healthcare22:107-113.
- BatraRK, KrishnanK, AgrawalA (2011) Paravertebral Block. J AnaesthesiolClinPharmacol27: 5-11.
- Naja MZ, Lonnqvist PA (2001) Somatic paravertebral nerve blockade: incidence of failed block and complications. Anaesthesia. 56: 1184-1188.
- Jadon A (2012) Nerve stimulator-guided thoracic paravertebral block for gynecomastia surgery. Indian J Anaesth 56:298-300.
- NikamS,Marghade P,Paliwal N,Lawhale (2014)S.Thoracic paravertebral block for breast surgery in a patient with ischemic heart disease. Anaesth,Pain and Intensive Care 18:280.
- Buckenmaier 3rd CC, Steele SM, Nielsen KC(2002)Para¬vertebral somatic nerve blocks for breast surgery in a pa¬tient with hypertrophic obstructive cardiomyopathy. Can J Anaesth49:571-574.
- Oğuz S, Küçük C, Eskiçirak E (2007) Thoracic paravertebral block or breast surgery in a patient with myasthenia gravis. J Anesth21:449-450.
- Park S, Kim Y, Han K(2010) Thoracic paravertebral block for breast surgery in a pregnant woman. Korean J Anesthesiol59:73-76.
- Exadaktylos AK, Buggy DJ, Moriarty DC (2006) Can anesthetic technique for primary breast cancer surgery affect re¬currence or metastasis? Anesthesiology105: 660-664.
- Poleshuck EL, Katz J, Andrus CH, Hogan LA, Jung BF, et al.(2006) Risk factors for chronic pain following breast cancer surgery: A prospective study. J Pain 7:626-634.
- Hura G, Knapik P, Misiołek H, Krakus A, Karpe J (2006) Sensory blockade after thoracic paravertebral injection of ropivacaine or bupivacaine. Eur J Anaesthesiol23: 658-664.
- YoshidaT, FujiwaraT, FarutaniK, OhashiN, BabaH(2014) Effects of ropivacaine concentration on the spread of sensory block produced by continuous thoracic paravertebral block: a prospective, randomised, controlled, double-blind study.Anaesthesia 69: 231-239.
- Mohamed SA, Fares KM, Mohamed AA, Alieldin NH (2014) Dexmedetomidine as an Adjunctive Analgesic with Bupivacaine in Paravertebral Analgesia for Breast Cancer Surgery Pain Physician 17:E589-E598.
- Pusch F,Wilding E,Klimscha W (2000) Sonographic measurement of needle insertion depth in paravertebral blocks in women.Br J Anaesth85:841-843.
- O Riain SC,Donnell BO, Cuffe T,Harmon DC,Fraher JP, et al. (2010) Thoracic paravertebral block using real-time ultrasound guidance.AnesthAnalg110:248-251.
- Votg A(2013)Paravertebral block –A new standard for perioperative analgesia. Trends in Anaesthesia and Critical Care 3:331-335.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences