Cast Wedging to Improve the Position of Fractures in Children: Too Painful and Outdated or Still a Viable Option?
Florian Freislederer, Thomas Erb, Tobias Berberich and Johannes Mayr
DOI10.36648/2471-982X.21.7.43
Florian Freislederer1*, Thomas Erb2, Tobias Berberich3 and Johannes Mayr1
1Department of Pediatric Surgery, University Children's Hospital Basel (UKBB), 4031 Basel, Switzerland
2Department of Pediatric Anesthesia, University Children's Hospital Basel (UKBB), University of Basel, 4056 Basel, Switzerland
3Department of Pediatric Surgery, St. Elisabethen Hospital, 79539 Lörrach, Germany
- *Corresponding Author:
- Florian Freislederer
Department of Pediatric Surgery
University Children's Hospital Basel (UKBB)
4031 Basel
Switzerland
Tel: +41799300992
E-mail: freislederer.florian@gmail.com
Received Date: April 23, 2021; Accepted Date: May 07, 2021; Published Date: May 14, 2021
Citation: Freislederer F, Erb T, Berberich T, Mayr J (2021) Cast Wedging to Improve the Position of Fractures in Children: Too Painful and Outdated or Still a Viable Option? Int J Anesth Pain Med Vol.7 No.3:43
Abstract
Tibial, forearm, and distal radius fractures are some of the most common types of fractures in children. If secondary loss of reduction results in angulation beyond the natural remodeling potential of the child's bone, conservative treatment options, including cast wedging, instead of closed/open reduction, are possible. The plaster wedge is an effective and child-friendly therapy for displaced bone fragments in forearm and lower leg fractures in the first 10 days after the fracture event.
The wedge procedure enables a gentle, closed reduction, which avoids the risk of sedation or surgical intervention and at the same time minimizes treatment costs. Complications are rare and can be easily corrected.
Keywords
Distal radius fractures; Sedation; Cast wedging; Persistent pain
Introduction
Cast wedging is a simple and non-invasive treatment method for secondary dislocated fractures of the long bones, which was described by Krömer and Heuritsch. Tibial, forearm, and distal radius fractures are some of the most common types of fractures in children. If secondary loss of reduction results in angulation beyond the natural remodeling potential of the child's bone, conservative treatment options, including cast wedging, instead of closed/open reduction, are possible. The plaster wedge is an effective and child-friendly therapy for displaced bone fragments in forearm and lower leg fractures in the first 10 days after the fracture event. The wedging procedure should be performed between the 6th and 10th day after the injury by cutting open the cast with a saw and bending it so that the fracture ends of the bone are better aligned again. A placeholder, e.g. pieces of cork, is inserted into the gap to stabilize the position of the fragments.
Cast Wedging
Up to the age of 12, most closed forearm and lower leg fractures can be treated with a cast without surgery if there is no rotational deformity, neurovascular impairment, or compartment syndrome. The loss of acceptable angulation after conservative treatment of forearm shaft fractures has been described in up to 39% [1]. The growing skeleton differs from the adult skeleton by a correction mechanism of the fractureinduced displacement [2]. Corrections of axial deviations in the frontal and sagittal planes are made in the periosteal-endosteal and epiphyseal regions of the bones. These corrections are particularly effective in the proximal humerus and distal forearm area. Ad latus shifts up to the width of the shaft are corrected by periosteal reshaping up to the age of 10 to 12 years. However, the proximal end of the radius is unable to adequately correct ad latus dislocations. In addition, spontaneous correction of rotational misalignment has only been demonstrated in fractures of the humerus and femur in young children [2-7]. Cast wedging is a simple and non-invasive treatment method for secondary dislocated fractures of the long bones, which was described by Krömer and Heuritsch as early as 1936 [1].
In principle, any axial deviation in the frontal and sagittal plane of the forearm or lower leg can be reduced by cast wedging so that the remaining angulation is within the limits of the spontaneous correction [2,5,6,8-11]. The wedging procedure should be performed between the 6th and 10th day after the injury by cutting open the cast with a saw and bending it so that the fracture ends of the bone are better aligned again. A placeholder, e.g. pieces of cork, is inserted into the gap to stabilize the position of the fragments. Performing the wedge procedure 6 to 10 days after the injury will allow the swelling of the tissue and thus the pain associated with correcting the bone deformity to be minimized.
Literature Review
Study results on cast wedging
Studies on cast wedging are sparse. A systematic literature search identified three studies that met strict criteria [1]. A total of 316 patients were included. The study design was prospective in one of the studies [10]; the other two studies did not provide any information about the study design. The average age of the patients included was between 7.1 and 9.3 years. The prospective study analyzed 48 forearm fractures of both bones and 22 fractures of the distal radius, nine of which were excluded due to a lack of radiological data [10]. Another study included 197 forearm and 52 lower leg fractures [9] and the third study only four forearm and two lower leg fractures. With regard to the results, the 2 studies, which included a considerable number of patients, were mainly discussed [9,10].
The prospective study used an angulation of >20° in each plane as a cut-off for cast wedging of the fractures of the distal radius, an angulation of >15° in each plane for fractures of the middle third of the forearm and for fractures of the proximal third of the forearm an angulation of >10° [10]. The other study established an angulation of >5° for the tibia and an angulation of >10° in the case of forearm fractures as an indication for the wedging of the cast [9]. The time of the plaster wedging (an average of ten days after the accident) and the duration of the immobilization (an average of 7.4 weeks) were only given in the latter study [9]. The patients were followed up for an average of 11.5 weeks and 18 weeks, respectively.
Wedge failure occurred in a total of 14 of 325 patients. Of these, three patients required surgical intervention; in 11 patients the healed deformity was left in place. Two unsatisfactory results after cast wedging of tibial fractures have been reported. One patient required surgical fixation and one patient showed residual varus alignment (of 6.6°). Eleven of 183 (6.01%) forearm fractures showed unsatisfactory results. Of these, one patient required surgical fixation and the deformity healed in ten patients. Further surgical fixation due to remaining unacceptable angulation after wedging (without specifying the fracture location) has been described. Eight patients also required remanipulation and a cast change (two tibia and six radius fractures).
The correction range after wedging the cast differed depending on the age of the patient and the location of the fracture. The improvement in coronary (i.e., anteroposterior (AP)) alignment was 4.4° to 8.3° and 3.0° to 4.7° for forearm and distal radius fractures and 4.1° for lower leg fractures, respectively. The improvement in sagittal (i.e., lateral) alignment was 6.3° to 12.1° and 13.9° to 15.7° for forearm and distal radius fractures and 1.8° for lower leg fractures, respectively.
In the prospective study, pain was reported in three of 61 patients after wedging and two of these patients experienced pain for up to two days after wedging the cast. This pain was described as mild and responded to over-the-counter analgesics, however this "mild" pain was not further described or measured. One patient showed temporary numbness of the fingers [10]. Overall, 4.4% of patients experienced wedge failure (requiring re-wedging, re-manipulation, and or surgery, or resulting in a healed deformity). The 95% CI for the total proportion was in the range from 2 to 6. There was no indication of a publication bias in the context of this systematic literature search [1].
In the literature, opening, closing and combined techniques of cast wedging are described, whereby the opening wedge technique, which is applied on the concave side of the fracture displacement, is the most common method due to its simple implementation. Accordingly, all of the above studies used an opening technique [9,10]. With opening and closing techniques, the pivot point is outside the extremity, while with the combined technique it is at fracture level. The question of the position of the wedge in relation to the break point continues to be debated. While some authors argue that the wedge should be placed directly at the fracture site, others prefer the wedge placement proximal to the fracture site (especially in distal fractures to ensure sufficient lever arm distal to the fracture) (Figure 1).
Figure 1: Cast wedging of a distal forearm fracture. (A): The wedge position is marked and the cast is cut approximately 2/3 of the circumference with an oscillating saw. (B): The cast can now be opened with a clamp until the desired correction is achieved. (C): The position is fixed using a placeholder (i.e., a piece of cork) and cotton wool is inserted at the wedge site to serve as a pillow. (D): The cast is stabilized with additional circular layers of synthetic cast.
To define angular deviations that require wedging, another paper combined literature data on forearm fracture patterns with expert opinions and introduced limits of acceptable angular deformities for different types of pediatric forearm fractures [12,13]. However, this study did not evaluate sagittal and coronary deformities separately. Von Laer defined the limit for spontaneous correction as an axial deviation of 10° in children aged 6 to 12 years for fractures of the proximal forearm shaft, 20° for greenwood fractures of the middle shaft, and complete fractures in children aged 3 to 5 years and 10° in children aged 6 to 12 years. For distal forearm fractures, von Laer set a limit of 10° in the frontal and 30° in the sagittal plane [5].
Pain during cast wedging
Usually, the pain associated with bone manipulation subsides within a few minutes. Although the current cast wedging therapy is associated with the use of non-opioid analgesics, minimal pain still occurs during the procedure, which is interpreted as a sign of bone movement and thus the success of the treatment. However, any pediatric treatment should be as painless as possible [14]. The contradiction of these principles has led to the controversial discussion of wedge therapy.
Since neither pain measurements during cast wedging therapy nor data on the effectiveness of the accompanying analgesic therapy are available in the literature, our working group carried out a prospective study that measured pain values (using the VAS scale according to Hicks) at several times during forearm cast wedging (Figure 1) under inhalation of nitrous oxide [15].
This international, bi-center, prospective observational study included 68 children (39 boys, 29 girls) aged 3 to 12 years (mean age 8 years, IQR age 4 years) with forearm fractures.
Patients between 3 to 12 years of age and in good physical condition (Class I or II according to the American Society of Anaesthesiologists Classification) were included.
The mean VAS value 5 minutes before wedging was 0 (IQR 0). This rose to a VAS value of 13-5 minutes after the inhalation of the nitrous oxide/oxygen mixture (IQR 2) was stopped. This difference was significant (p=0.015).
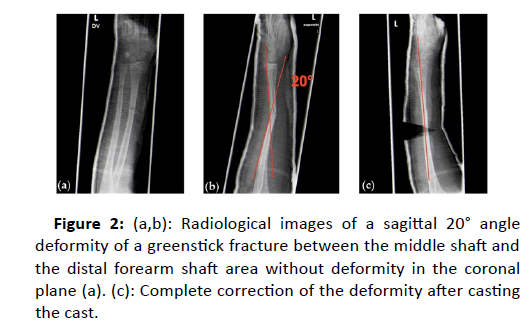
The mean VAS value for the maximum pain that was remembered 30 minutes after the end of the inhalation of the nitrous oxide/oxygen mixture was 0 (IQR 1). One patient (1.5% of the patients) complained a VAS value >4 (VAS 6) 3-5 minutes after the end of inhalation of the nitrous oxide/oxygen mixture. The pain decreased to below 4 after oral administration of ibuprofen. Another 2 (2.9%) patients reported a VAS value of 6 for the maximum pain they could remember. However, these patients did not have a VAS value >4, measured 3-5 minutes after the wedging procedure (Figure 2).
5 of 15 (33.3%) patients with significant displacement of bone fragments with a total angle correction of >15° by cast wedging reported a VAS value of ≥ 4, 3-5 minutes after the end of the nitrous oxide/oxygen inhalation.
The maximum recalled pain recorded 30 minutes after the end of the inhalation fell to ≤ 2 in 12 of these 15 (80%) patients. The remaining three patients reported a VAS value of 30 minutes after the end of the nitrous oxide/oxygen inhalation ≤ 4.
After wedging, we did not see any failure of the angle correction. However, a patient's cast had to be replaced one day after the wedge procedure due to persistent pain, which resolved the issue and the patient was not further followed-up in the study. There were no further complications.
In our study we achieved a mean correction of the total angular deformity of 10. In 7/68 (10%) patients only a minimal correction (≤ 3) was achieved.
Bone healing with cast treatment in children is not a static process and changes in orientation can occur over time once the tissue swelling decreases, especially if the immobilization position has not been corrected or changed. Therefore, even a small correction of the angulation during the first 2 weeks after the injury can be the decisive factor for fracture healing with acceptable alignment of the bone fragments.
Discussion and Conclusion
In summary, cast wedging is an effective and child-friendly therapy for displaced bone fragments in forearm and lower leg fractures in the first 10 days after the fracture event.
Despite the current trend towards surgical treatment of forearm fractures in children in developed countries, cast wedging is a reliable, non-invasive method in the pediatric population that is successful approximately 96% of the time. The wedge procedure enables a gentle, closed reduction, which avoids the risk of sedation or surgical intervention and at the same time minimizes treatment costs. Complications are rare and can be easily corrected. The degree of correction after wedging appears to be greatest in fractures of the distal radius in the sagittal plane (approx. 15°) and lowest in fractures of the lower leg in the sagittal plane (approx. 2°). Due to the limited amount of data available, further studies evaluating cast wedging are needed.
References
- Gaukel S, Leu S, Fink L, Skovgaard SR, Ramseier LE, et al. (2017) Cast wedging: A systematic review of the present evidence. J Child Orthop 11: 398-403.
- Checo F (2009) Pediatric Forearm Fractures. Journal of Chromesthesia 24: 163-171.
- Luther G, Patricia M, Peter MW, Donald SB (2016) Radiographic evaluation during treatment of pediatric forearm fractures:Implications on clinical care and costs. J Pediatr Orthop 36 :465-471.
- Ploss C, Marzi I (2016) Pediatric Traumatology.
- Von LL (2007) Fractures and dislocations in growing age.
- Weinberg AM. Upper extremity fractures in children, part II: Radial head, olecranon, forearm, hand. Orthopedics and trauma surgery update 3: 21-40.
- Wilkins KE (2005) Principles of fracture remodeling in children. Injury. 36: A3-A11.
- Bebbington A, Lewis P, Savage R (2005) Cast wedging for orthopaedic surgeons. Injury 36: 71-72.
- Kattan JM, Leathers MP, Barad JH, Silva M (2014) The effectiveness of cast wedging for the treatment of pediatric fractures. J Pediatr Orthop B 23: 566-571
- Samora JB, Balch JS, Kevin EK, Allan CB, John RK, et al. (2014) Is there still a place for cast wedging in pediatric forearm fractures? J Pediatr Orthop 34: 246-252.
- Wells L, Avery LA, Hosalkar HH, Friedman EJ, Davidson SR (2010) Cast Wedging: A “forgotten” yet predictable method for correcting fracture deformity. University of Pennsylvania Orthopaedic Journal 20: 113-116.
- Berberich T, Reimann P, Steinacher M, Erb TO, Mayr J (2008) Evaluation of cast wedging in a forearm fracture model. Clin Biomech 23: 895-899.
- Ploegmakers JW, Cees V (2006) Acceptance of angulation on the non-operative treatment of paediatric forearm fractures. J Pediatr Orthop 15: 428-432.
- Ireland (2012) Good practice in postoperative and procedural pain management. Pediatric Anesthesia.
- Freislederer F, Berberich T, Erb TO, Mayr J (2020) Pain during cast wedging of forearm shaft and distal forearm fractures in children aged 3 to 12 years-A prospective, observational study. Children 7: 229.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences